Healthcare perspectives from The Economist Intelligence Unit
Covid-19: tracking the pandemic
17384
Related content
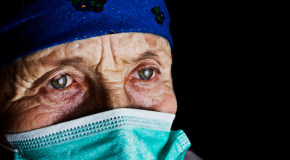
Covid-19: the greatest burden will fall on older people in low- and middle-...
We are living in unprecedented times. The covid-19 pandemic is escalating rapidly with more than 173, 300 confirmed cases and over 7,000 deaths in 152 countries and regions (see Figure 1). The majority of cases and deaths are among people aged 60 years and older living in low- and middle-income countries (LMICs) where healthcare resources to treat people and control the epidemic are limited.
Guidance largely ignores this issue in both high income countries (HICs) and LMICS, the latter of which contain 69% of the global population aged 60 years and over. Their health systems are also weaker, leaving them vulnerable to the worst impacts of covid-19. Limited guidance which is more relevant to HICs has been produced for older people but not for health and social care workers, care homes or day centres. No detailed age-specific data on global cases and mortality has been produced by the World Health Organisation (WHO) even though mortality rates jump sharply in older people, rising from 8% in those aged 70 to 79 years to 15% in those aged 80 and over (see Figure 2 which shows the effect of age on risk of dying from covid-19 from the Chinese outbreak).
In the absence of clear comprehensive guidelines for prevention and control of covid-19 among older people, ad hoc policies are emerging. In Italy scarce hospital and intensive care services are being prioritised for younger, otherwise healthy patients over older patients, according to reports. In the UK, people aged 70 and over will be expected to self-isolate themselves for up to four months in the coming weeks.
In LMICs, older people provide an integral economic and social resource to societies, including bringing up grandchildren to support the labour mobility of their adult children and relatives. Beyond grief and bereavement the implications of covid-19 deaths among the older population will be profound, especially when family members working abroad are unable to return home at short notice.
Increasing numbers of very old people are now being cared for in nursing homes in LMICs. These homes are often unregulated, provide care of very poor quality and may even act as incubators of infection (as do cruise ships, prisons, mines and HIC nursing homes). Outbreaks in LMIC institutions would have serious implications, further underpinning the need for international guidance similar to that issued recently by the International Federation of the Red Cross and Red Crescent Societies, UNICEF and the WHO regarding children and schools.
The ability of health systems to cope with a surge in demand is extremely limited, especially for patients needing intensive care. Health systems in LMICs face severe constraints on capacity at normal times and are unlikely to be able to keep up, especially if the precarious staffing levels—already depleted by migration, low salaries and poor working conditions—and limited gerontological expertise are reduced further by illness. The needs of older people are not being adequately addressed in developing covid-19 policy and practice. Current social distancing policies ignore the precarious existence of many older people and fail to account for the realities faced by those living alone and individuals who are dependent on others. The high levels of illiteracy in LMICs also present a challenge which has yet to be considered in any meaningful way.
An age perspective needs to be explicitly included in the development of national and global planning for covid-19, and it is increasingly clear that a global expert group should be formed to provide support and guidance for older people, home carers, residential facilities and overburdened hospitals in LMICs.
Shah Ebrahim is an honorary professor of public health at the London School of Hygeine & Tropical Medicine. He would like to thank Peter Lloyd- Sherlock, professor of social policy and international development, University of East Anglia; Leon Geffen, Samson Institute for Ageing Research, Cape Town, South Africa; and Martin McKee, professor of European public health, London School of Hygiene & Tropical Medicine, for contributing to this article. The views and opinions expressed in this article are those of the author(s) and do not necessarily reflect the views of The Economist Group or any of its affiliates. The Economist Group cannot accept any responsibility or liability for reliance by any person on this article or any of the information, opinions or conclusions set out in the article.

The secret life of coronavirus: Why we need such drastic social distancing...
Left unchecked, the novel coronavirus (covid-19) will continue to sweep the globe. The horror stories from emergency departments and initial estimates of fatality rates starkly portend large numbers of people dying from both the virus and insufficient healthcare capacity. However, there is disagreement about what it will take to halt this progression and how far our preventative measures should go.
Our analysis in early February of 458 confirmed covid-19 cases across 93 Chinese cities was one of the clear early warnings that without interventions the average time between successive cases in a transmission chain is less than a week (around four days). Moreover, people can spread covid-19 before they even know they are sick, and there are individuals known as “super-spreaders” who infect an unusually large number of others.
These data help us understand why covid-19 is measurably more difficult to contain than a similar virus, SARS (severe acute respiratory syndrome). It comes down to a race between humans and the virus—how rapidly we can track down an infected person’s contacts versus how quickly the viral infection can incubate and spread.
While covid-19 moves quickly and sometimes silently, SARS is slow and visible. The serial interval of each demonstrates why covid-19 is the more insidious threat: if person A infects person B, the serial interval is the time between person A developing symptoms and person B developing symptoms. SARS has a serial interval of around eight days—twice as long as covid-19—and no pre-symptomatic transmission.
Imagine that a patient is diagnosed with SARS two days after first feeling sick. Public health authorities would have time on their side, perhaps a full six days to track down and isolate anyone who had contact with the patient over the prior two days. With covid-19, by the time of diagnosis a patient may have already been contagious for several days. During this period they may have infected many others who are also now spreading the virus—possibly without displaying any symptoms.
This is why covid-19 requires more drastic measures than SARS. It can spread quickly and silently, and we cannot possibly identify every infectious individual in an emerging outbreak, particularly with limited laboratory-testing capacity.
Super-spreading events compound the challenge. Among the 458 Chinese cases, five people infected over five others, with the biggest super-spreader infecting at least 16 people. Network theory—the mathematics that underlies the computer models that predict how the disease will spread— tells us that even a few people capable of infecting large numbers of others can dramatically amplify transmission and undermine interventions.
The recent threats of SARS, swine flu, Ebola, and Zika have brought fame to an epidemiological statistic known as R0. It stands for the basic reproduction number and is intended to be an indicator of the contagiousness of infectious agents (it is pronounced R-naught). In short it tells us how many people each new case will infect during the early days of a pandemic on average. An outbreak is expected to continue if R0 has a value >1 and to end if R0 is <1.
A lot of attention has been paid to recent estimates suggesting that covid-19 has a lower R0 than SARS, roughly two versus three. Clearly, then, R0 is not the whole story. It indicates whether one case will turn into two or three or four, but not how quickly or how silently that will come to pass.
The level of intervention required to curb an outbreak very much depends on all three factors: its R0 value, speed, and visibility in the community. We should not be fooled by the relatively modest R0 of covid-19 as its speed and stealth make it all the more difficult to contain. Even if each case infects only two others, the number of infections can skyrocket undetected in the absence of early and extensive control measures that limit person-to-person contact.
Our study highlights the elusiveness of covid-19. Keeping people apart is the only guaranteed way to block infections given the immense challenge of identifying contagious and soon-to-be contagious cases. Whether the policy goal is to stop transmission, protect those at high risk, or "flatten the curve" to ensure that fewer people are sick at any one time, extreme social distancing strategies of the type we have been seeing are strongly recommended.
Professor Lauren Ancel Meyers is the Cooley Centennial Professor of biology and statistics at the University of Texas at Austin, where she develops powerful mathematical methods for forecasting the spread of diseases and designing effective disease control strategies. The views and opinions expressed in this article are those of the author(s) and do not necessarily reflect the views of The Economist Group or any of its affiliates. The Economist Group cannot accept any responsibility or liability for reliance by any person on this article or any of the information, opinions or conclusions set out in the article.

Covid-19 pandemic accelerates the rise of digital payments
China, South Korea and the US Federal Reserve have started quarantining or disinfecting banknotes. It is well-known that currency in circulation can serve as a vehicle for transmitting pathogens, though the potency of pathogens transmitted via cash remains unclear. The human influenza virus, for example, can remain alive and infectious for more than two weeks on banknotes. Although it’s not known whether the exchange of currency infected with influenza can dramatically increase its spread, responses from the US, Korean and Chinese governments raise concerns.
It’s possible that these governments are simply taking extreme precautionary measures. It’s also possible that physical currency can indeed be a significant transmission medium for highly infectious diseases such as covid-19. A local branch of the People's Bank of China in Guangzhou has even opted to destroy banknotes that have been in circulation in high-risk settings such as hospitals or wet-markets.
These measures reflect earlier governmental responses to infectious disease. A late 1940s report on Egypt’s cholera epidemic highlighted the viability of cholera pathogens on banknotes. Throughout history people have responded to sickness in a similar way by washing or fumigating banknotes, yet we still have limited understanding of how physical currencies might transmit new pathogens.
There’s no doubt that covid-19 will accelerate the pre-existing trend towards digital payments in Asia, and China in particular. In late October 2019, Chinese President Xi Jinping endorsed blockchain—a digital ledger technology on which digital currencies can be transacted—as “an important breakthrough for independent innovation of core technologies”. He added that the People’s Bank of China intended to replace cash with a government-issued digital currency. The Chinese government actively promotes its internet banking infrastructure, whereas Western nations rarely use a top-down approach to governance.
In China, where digital payments are already prevalent, covid-19 could be a significant driver for the total elimination of cash. In 2018, nearly 73% of Chinese internet users made online payments (up from 18% in 2008). According to a recent survey by Deutsche Bank, this increase is partly driven by young people who are typically more open to adopting new technologies. China and Southeast Asian countries have much larger young populations than Europe and the US.
Western countries have tended to move at a slower pace towards digital payments than, for example, China. Part of the reason for this lies, according to Deutsche Bank, in different payment cultures of countries. A third of the people in OECD countries consider cash to be their favourite payment method, and more than half believe cash will always be around. Citizens in many European countries (notably Germany) and those in the US have a marked preference for cash.
Source: Deutsche Bank, The Future of Payments.
But even in Western countries that share similar payment cultures we can observe variation in digital preparedness. In terms of homegrown fintech champions that could benefit most from a digital payments transition, Europe’s are much smaller in size than large US counterparts such as Apple Pay, Google Pay, and PayPal—to name a few. Beyond that, many of Europe’s leading digital payment service companies are controlled or backed by US and Chinese companies (eg Swedish financial technology company IZettle was recently acquired by PayPal and Germany’s mobile N26 bank is backed by China’s Tencent).
Nonetheless, European countries are determined to be at the forefront of digital currencies. Central banks such as the Bank of England, the European Central Bank, the Swiss National Bank and the Swedish Riksbank have started to assess the feasibility of digital central bank currencies. These would perform all the functions of banknotes and coins and could then be used by households and businesses to make both payments and savings. The transition will not be easy. Digital central bank currencies require infrastructure that can record in-person and online transactions, which means that governments will need private sector co-operation.
Under “normal” conditions it would take a long time to change culturally ingrained habits and institutional legacies related to long and well-established payments systems. Jodie Kelley—CEO of the US Electronic Transactions Association—said in a recent interview that “people default to what’s familiar, unless there’s something to jolt you out of it”. She continued that “contactless payments have come up as a new option for consumers who are much more conscious of what they touch”.
The covid-19 pandemic could move the world more rapidly towards digital payments. In France, the Louvre museum in Paris recently banned cash due to covid-19 fears. The museum did this even though its policy clashes with the Bank of France's requirement that all businesses accept cash.
It is too early to conclude what the changes might look like in each cultural, demographic, and institutional context, but we can be sure that covid-19 is already reinforcing existing trends towards increased digitisation of payments.
Dr Marion Laboure and Sachin Silva are the co-authors of this blog. Marion Laboure is a macro strategist at Deutsche Bank and Sachin Silva is a doctoral candidate and fellow at Harvard University specialising in global health and economics.
The views and opinions expressed in this article are those of the author(s) and do not necessarily reflect the views of The Economist Group or any of its affiliates. The Economist Group cannot accept any responsibility or liability for reliance by any person on this article or any of the information, opinions or conclusions set out in the article.
The secret life of coronavirus: Why we need such drastic social distancing measures
Related content

Value-based healthcare in Sweden: Reaching the next level
The need to get better value from healthcare investment has never been more important as ageing populations and increasing numbers of people with multiple chronic conditions force governments to make limited financial resources go further.
These pressures, along with a greater focus on patient-centred care, have raised the profile of VBHC, especially in European healthcare systems. Sweden, with its highly comprehensive and egalitarian healthcare system, has been a leader in implementing VBHC from the beginning, a fact that was underscored in a 2016 global assessment of VBHC published by The Economist Intelligence Unit.
This paper looks at the ways in which Sweden has implemented VBHC, the areas in which it has faced obstacles and the lessons that it can teach other countries and health systems looking to improve the value of their own healthcare investments.

Breast cancer patients and survivors in the Asia-Pacific workforce
With more older women also working, how will the rising trend of breast cancer survivorship manifest in workplace policies, practices and culture? What challenges do breast cancer survivors face when trying to reintegrate into the workforce, or to continue working during treatment? How can governments, companies and society at large play a constructive role?
This series of reports looks at the situation for breast cancer survivors in Australia, New Zealand and South Korea. It finds that while progress has been made, more needs to be done, particularly in South Korea, where public stigma around cancer remains high.
The Cost of Silence
Cardiovascular diseases levy a substantial financial toll on individuals, their households and the public finances. These include the costs of hospital treatment, long-term disease management and recurring incidence of heart attacks and stroke. They also include the costs of functional impairment and knock-on costs as families may lose breadwinners or have to withdraw other family members from the workforce to care for a CVD patient. Governments also lose tax revenue due to early retirement and mortality, and can be forced to reallocate public finances from other budgets to maintain an accessible healthcare system in the face of rising costs.
As such, there is a need for more awareness of the ways in which people should actively work to reduce their CVD risk. There is also a need for more primary and secondary preventative support from health agencies, policymakers and nongovernmental groups.
To inform the decisions and strategies of these stakeholders, The Economist Intelligence Unit and EIU Healthcare, its healthcare subsidiary, have conducted a study of the prevalence and costs of the top four modifiable risk factors that contribute to CVDs across the Asian markets of China, Australia, Hong Kong, Japan, Singapore, South Korea, Taiwan and Thailand.
Download the report to learn more.
Covid-19 pandemic accelerates the rise of digital payments
Related content

Covid-19: the greatest burden will fall on older people in low- and middle-...
We are living in unprecedented times. The covid-19 pandemic is escalating rapidly with more than 173, 300 confirmed cases and over 7,000 deaths in 152 countries and regions (see Figure 1). The majority of cases and deaths are among people aged 60 years and older living in low- and middle-income countries (LMICs) where healthcare resources to treat people and control the epidemic are limited.
Guidance largely ignores this issue in both high income countries (HICs) and LMICS, the latter of which contain 69% of the global population aged 60 years and over. Their health systems are also weaker, leaving them vulnerable to the worst impacts of covid-19. Limited guidance which is more relevant to HICs has been produced for older people but not for health and social care workers, care homes or day centres. No detailed age-specific data on global cases and mortality has been produced by the World Health Organisation (WHO) even though mortality rates jump sharply in older people, rising from 8% in those aged 70 to 79 years to 15% in those aged 80 and over (see Figure 2 which shows the effect of age on risk of dying from covid-19 from the Chinese outbreak).
In the absence of clear comprehensive guidelines for prevention and control of covid-19 among older people, ad hoc policies are emerging. In Italy scarce hospital and intensive care services are being prioritised for younger, otherwise healthy patients over older patients, according to reports. In the UK, people aged 70 and over will be expected to self-isolate themselves for up to four months in the coming weeks.
In LMICs, older people provide an integral economic and social resource to societies, including bringing up grandchildren to support the labour mobility of their adult children and relatives. Beyond grief and bereavement the implications of covid-19 deaths among the older population will be profound, especially when family members working abroad are unable to return home at short notice.
Increasing numbers of very old people are now being cared for in nursing homes in LMICs. These homes are often unregulated, provide care of very poor quality and may even act as incubators of infection (as do cruise ships, prisons, mines and HIC nursing homes). Outbreaks in LMIC institutions would have serious implications, further underpinning the need for international guidance similar to that issued recently by the International Federation of the Red Cross and Red Crescent Societies, UNICEF and the WHO regarding children and schools.
The ability of health systems to cope with a surge in demand is extremely limited, especially for patients needing intensive care. Health systems in LMICs face severe constraints on capacity at normal times and are unlikely to be able to keep up, especially if the precarious staffing levels—already depleted by migration, low salaries and poor working conditions—and limited gerontological expertise are reduced further by illness. The needs of older people are not being adequately addressed in developing covid-19 policy and practice. Current social distancing policies ignore the precarious existence of many older people and fail to account for the realities faced by those living alone and individuals who are dependent on others. The high levels of illiteracy in LMICs also present a challenge which has yet to be considered in any meaningful way.
An age perspective needs to be explicitly included in the development of national and global planning for covid-19, and it is increasingly clear that a global expert group should be formed to provide support and guidance for older people, home carers, residential facilities and overburdened hospitals in LMICs.
Shah Ebrahim is an honorary professor of public health at the London School of Hygeine & Tropical Medicine. He would like to thank Peter Lloyd- Sherlock, professor of social policy and international development, University of East Anglia; Leon Geffen, Samson Institute for Ageing Research, Cape Town, South Africa; and Martin McKee, professor of European public health, London School of Hygiene & Tropical Medicine, for contributing to this article. The views and opinions expressed in this article are those of the author(s) and do not necessarily reflect the views of The Economist Group or any of its affiliates. The Economist Group cannot accept any responsibility or liability for reliance by any person on this article or any of the information, opinions or conclusions set out in the article.

Beyond Cash: China’s Emerging Payments Market
As China’s economy continues its robust expansion, and as its banking sector finally opens up to foreign competition, the demand for credit is taking off. Local banks have ramped up their operations for the last three or four years in preparation for increased competition from foreign rivals. As their efforts bear fruit, the potential for China’s payment cards market has never looked better.
Nowhere is this more so than in China’s emerging market for debit and credit cards. With more than 200m new cards issued last year alone, China’s total number of plastic cards broke though the one billion mark in 2006, with no sign of the pace abating. While a relatively tiny portion of this total—some 50 million—are currently credit cards, growth rates for the sector (both in terms of spending and transaction volumes) are now much higher than for the mass-market debit cards that form the bulk of cards in circulation. No surprise, then, that foreign banks are now eyeing this space for opportunity.
The main findings of our research are as follows:
Retail banks are very bullish on consumer banking in general—and credit cards in particular... For many of the retail banks surveyed for this report, credit cards are the main priority. When asked what products they believe hold the greatest prospects for China’s personal banking industry, retail bankers were most optimistic about credit cards and bank accounts. Fifty-fivepercent of study respondents believe the prospects for these consumer banking products are ‘highly promising’ over the next three years. Debit cards are seen as the next most promising item (45%), although these are directly linked to the prospects for basic bank accounts, followed by wealth and investment management (40%). In fact, respondents report overwhelmingly positive views for all aspects of the consumer banking sector. ...But the outlook for profits is less certain. When it comes to profits in the credit card market, our survey respondents are less confident. Forty-three percent agree that it would be difficult to make a profit in the credit card market over the next three years, compared with 36% who remain uncertain and just 21% who believe it is possible. The key issue is tough competition for customers between local banks growing their market share and foreign rivals trying to establish a beach head in China. This competition inevitably leads to lower card fees, which keeps earnings low (or negative). In addition, banks are grappling with low rates of revolving credit on cards, resulting from a cultural aversion to accruing debt, together with low fees and interest rates that issuers are allowed to levy on merchants and card users. Infrastructure is key to growth in the cards market. According to the executives surveyed for this report, improving infrastructure – encompassing both merchants and ATMs—will play the biggest role in encouraging the increased acceptance of card payments in China. Fully 83% of retail bankers polled chose this as an essential requirement. This component scores far ahead of any other criteria, for example better collaboration between key stakeholders such as banks and payment processors (48%) or publicity campaigns (33%). When asked what the Chinese market needs to supporta payments infrastructure, half of the survey respondents selected better availability of consumer credit-history data. Merchant acquisition is a major hurdle. Convincing merchants to accept credit cards is a major challenge for banks. Eight out of ten retail bankers polled for this report say that local retailers’ preference for cash is either a ‘very significant’ or ‘significant’ barrier in operating cards and payment services. In part, this is because retailers don’t yet feel much pressure from customers to provide payment card facilities in a society where cash is traditionally preferred. Despite an opening financial market, much risk remains. More than half (53%) of bankers polled for this report selected political risk, relating to policy and regulation, as the biggest existing or potential risk associated with their firm’soperations in China. Retail bankers in particular listed licensing risk (chosen by 43%) as a major concern, second only to political risk, highlighting the difficulties associated with getting permission to expand into new regions or markets. Along with this, 41% of the respondents expressed a general concern about the outlook for China’s banking industry.Much work needs to be done to promote a plastic card payment culture in China. More than anything else, a more extensive card network and infrastructure must be rolled out to promote consumer usage. Along with this, databases of consumers’ credit and transaction histories require expansion. In addition, Chinese consumers must be encouraged to make the switch from cash-based transactions to plastic cards. Despite these challenges, growth is already strong. And in cities such as Beijing, efforts to prepare for the 2008 Summer Olympic Games will help create an environment that supports card payments. Although foreign banks entering the market will have their work cut out, the opportunity is simply too big to ignore.

Value-based healthcare in Sweden: Reaching the next level
The need to get better value from healthcare investment has never been more important as ageing populations and increasing numbers of people with multiple chronic conditions force governments to make limited financial resources go further.
These pressures, along with a greater focus on patient-centred care, have raised the profile of VBHC, especially in European healthcare systems. Sweden, with its highly comprehensive and egalitarian healthcare system, has been a leader in implementing VBHC from the beginning, a fact that was underscored in a 2016 global assessment of VBHC published by The Economist Intelligence Unit.
This paper looks at the ways in which Sweden has implemented VBHC, the areas in which it has faced obstacles and the lessons that it can teach other countries and health systems looking to improve the value of their own healthcare investments.
Covid-19: the greatest burden will fall on older people in low- and middle-income countries
Related content

Value-based healthcare in Sweden: Reaching the next level
The need to get better value from healthcare investment has never been more important as ageing populations and increasing numbers of people with multiple chronic conditions force governments to make limited financial resources go further.
These pressures, along with a greater focus on patient-centred care, have raised the profile of VBHC, especially in European healthcare systems. Sweden, with its highly comprehensive and egalitarian healthcare system, has been a leader in implementing VBHC from the beginning, a fact that was underscored in a 2016 global assessment of VBHC published by The Economist Intelligence Unit.
This paper looks at the ways in which Sweden has implemented VBHC, the areas in which it has faced obstacles and the lessons that it can teach other countries and health systems looking to improve the value of their own healthcare investments.

Breast cancer patients and survivors in the Asia-Pacific workforce
With more older women also working, how will the rising trend of breast cancer survivorship manifest in workplace policies, practices and culture? What challenges do breast cancer survivors face when trying to reintegrate into the workforce, or to continue working during treatment? How can governments, companies and society at large play a constructive role?
This series of reports looks at the situation for breast cancer survivors in Australia, New Zealand and South Korea. It finds that while progress has been made, more needs to be done, particularly in South Korea, where public stigma around cancer remains high.
The Cost of Silence
Cardiovascular diseases levy a substantial financial toll on individuals, their households and the public finances. These include the costs of hospital treatment, long-term disease management and recurring incidence of heart attacks and stroke. They also include the costs of functional impairment and knock-on costs as families may lose breadwinners or have to withdraw other family members from the workforce to care for a CVD patient. Governments also lose tax revenue due to early retirement and mortality, and can be forced to reallocate public finances from other budgets to maintain an accessible healthcare system in the face of rising costs.
As such, there is a need for more awareness of the ways in which people should actively work to reduce their CVD risk. There is also a need for more primary and secondary preventative support from health agencies, policymakers and nongovernmental groups.
To inform the decisions and strategies of these stakeholders, The Economist Intelligence Unit and EIU Healthcare, its healthcare subsidiary, have conducted a study of the prevalence and costs of the top four modifiable risk factors that contribute to CVDs across the Asian markets of China, Australia, Hong Kong, Japan, Singapore, South Korea, Taiwan and Thailand.
Download the report to learn more.
What can we do about the childhood cancers never diagnosed or treated?
Over the next ten years we can look forward to seeing an additional 1m children surviving cancer around the world. This success story will be achieved through the concerted efforts of multiple agencies to support implementation of the World Health Organisation’s global initiative for childhood cancer. This was announced in 2018 and aims to increase survival rates to at least 60% by 2030.
17350
Related content

Value-based healthcare in Sweden: Reaching the next level
The need to get better value from healthcare investment has never been more important as ageing populations and increasing numbers of people with multiple chronic conditions force governments to make limited financial resources go further.
These pressures, along with a greater focus on patient-centred care, have raised the profile of VBHC, especially in European healthcare systems. Sweden, with its highly comprehensive and egalitarian healthcare system, has been a leader in implementing VBHC from the beginning, a fact that was underscored in a 2016 global assessment of VBHC published by The Economist Intelligence Unit.
This paper looks at the ways in which Sweden has implemented VBHC, the areas in which it has faced obstacles and the lessons that it can teach other countries and health systems looking to improve the value of their own healthcare investments.

Breast cancer patients and survivors in the Asia-Pacific workforce
With more older women also working, how will the rising trend of breast cancer survivorship manifest in workplace policies, practices and culture? What challenges do breast cancer survivors face when trying to reintegrate into the workforce, or to continue working during treatment? How can governments, companies and society at large play a constructive role?
This series of reports looks at the situation for breast cancer survivors in Australia, New Zealand and South Korea. It finds that while progress has been made, more needs to be done, particularly in South Korea, where public stigma around cancer remains high.
The Cost of Silence
Cardiovascular diseases levy a substantial financial toll on individuals, their households and the public finances. These include the costs of hospital treatment, long-term disease management and recurring incidence of heart attacks and stroke. They also include the costs of functional impairment and knock-on costs as families may lose breadwinners or have to withdraw other family members from the workforce to care for a CVD patient. Governments also lose tax revenue due to early retirement and mortality, and can be forced to reallocate public finances from other budgets to maintain an accessible healthcare system in the face of rising costs.
As such, there is a need for more awareness of the ways in which people should actively work to reduce their CVD risk. There is also a need for more primary and secondary preventative support from health agencies, policymakers and nongovernmental groups.
To inform the decisions and strategies of these stakeholders, The Economist Intelligence Unit and EIU Healthcare, its healthcare subsidiary, have conducted a study of the prevalence and costs of the top four modifiable risk factors that contribute to CVDs across the Asian markets of China, Australia, Hong Kong, Japan, Singapore, South Korea, Taiwan and Thailand.
Download the report to learn more.
How society needs to revamp food packaging to beat obesity
Related content

Value-based healthcare in Sweden: Reaching the next level
The need to get better value from healthcare investment has never been more important as ageing populations and increasing numbers of people with multiple chronic conditions force governments to make limited financial resources go further.
These pressures, along with a greater focus on patient-centred care, have raised the profile of VBHC, especially in European healthcare systems. Sweden, with its highly comprehensive and egalitarian healthcare system, has been a leader in implementing VBHC from the beginning, a fact that was underscored in a 2016 global assessment of VBHC published by The Economist Intelligence Unit.
This paper looks at the ways in which Sweden has implemented VBHC, the areas in which it has faced obstacles and the lessons that it can teach other countries and health systems looking to improve the value of their own healthcare investments.

Breast cancer patients and survivors in the Asia-Pacific workforce
With more older women also working, how will the rising trend of breast cancer survivorship manifest in workplace policies, practices and culture? What challenges do breast cancer survivors face when trying to reintegrate into the workforce, or to continue working during treatment? How can governments, companies and society at large play a constructive role?
This series of reports looks at the situation for breast cancer survivors in Australia, New Zealand and South Korea. It finds that while progress has been made, more needs to be done, particularly in South Korea, where public stigma around cancer remains high.
The Cost of Silence
Cardiovascular diseases levy a substantial financial toll on individuals, their households and the public finances. These include the costs of hospital treatment, long-term disease management and recurring incidence of heart attacks and stroke. They also include the costs of functional impairment and knock-on costs as families may lose breadwinners or have to withdraw other family members from the workforce to care for a CVD patient. Governments also lose tax revenue due to early retirement and mortality, and can be forced to reallocate public finances from other budgets to maintain an accessible healthcare system in the face of rising costs.
As such, there is a need for more awareness of the ways in which people should actively work to reduce their CVD risk. There is also a need for more primary and secondary preventative support from health agencies, policymakers and nongovernmental groups.
To inform the decisions and strategies of these stakeholders, The Economist Intelligence Unit and EIU Healthcare, its healthcare subsidiary, have conducted a study of the prevalence and costs of the top four modifiable risk factors that contribute to CVDs across the Asian markets of China, Australia, Hong Kong, Japan, Singapore, South Korea, Taiwan and Thailand.
Download the report to learn more.
Moving Universal Health Coverage from Ambition to Practice
Executive Summary
Universal Health Coverage (UHC) is one of the health targets within the sustainable development goals (SDGs). It means that everyone who needs healthcare services receives ones of sufficient quality without having to experience financial hardship. Reaching this goal is a task both large and urgent: currently more than a half of the world’s population lack access to at least some essential element of healthcare.
17324
Related content

Value-based healthcare in Sweden: Reaching the next level
The need to get better value from healthcare investment has never been more important as ageing populations and increasing numbers of people with multiple chronic conditions force governments to make limited financial resources go further.
These pressures, along with a greater focus on patient-centred care, have raised the profile of VBHC, especially in European healthcare systems. Sweden, with its highly comprehensive and egalitarian healthcare system, has been a leader in implementing VBHC from the beginning, a fact that was underscored in a 2016 global assessment of VBHC published by The Economist Intelligence Unit.
This paper looks at the ways in which Sweden has implemented VBHC, the areas in which it has faced obstacles and the lessons that it can teach other countries and health systems looking to improve the value of their own healthcare investments.

Breast cancer patients and survivors in the Asia-Pacific workforce
With more older women also working, how will the rising trend of breast cancer survivorship manifest in workplace policies, practices and culture? What challenges do breast cancer survivors face when trying to reintegrate into the workforce, or to continue working during treatment? How can governments, companies and society at large play a constructive role?
This series of reports looks at the situation for breast cancer survivors in Australia, New Zealand and South Korea. It finds that while progress has been made, more needs to be done, particularly in South Korea, where public stigma around cancer remains high.
The Cost of Silence
Cardiovascular diseases levy a substantial financial toll on individuals, their households and the public finances. These include the costs of hospital treatment, long-term disease management and recurring incidence of heart attacks and stroke. They also include the costs of functional impairment and knock-on costs as families may lose breadwinners or have to withdraw other family members from the workforce to care for a CVD patient. Governments also lose tax revenue due to early retirement and mortality, and can be forced to reallocate public finances from other budgets to maintain an accessible healthcare system in the face of rising costs.
As such, there is a need for more awareness of the ways in which people should actively work to reduce their CVD risk. There is also a need for more primary and secondary preventative support from health agencies, policymakers and nongovernmental groups.
To inform the decisions and strategies of these stakeholders, The Economist Intelligence Unit and EIU Healthcare, its healthcare subsidiary, have conducted a study of the prevalence and costs of the top four modifiable risk factors that contribute to CVDs across the Asian markets of China, Australia, Hong Kong, Japan, Singapore, South Korea, Taiwan and Thailand.
Download the report to learn more.
Antimicrobial resistance and climate change: Two wicked problems
Related content

Value-based healthcare in Sweden: Reaching the next level
The need to get better value from healthcare investment has never been more important as ageing populations and increasing numbers of people with multiple chronic conditions force governments to make limited financial resources go further.
These pressures, along with a greater focus on patient-centred care, have raised the profile of VBHC, especially in European healthcare systems. Sweden, with its highly comprehensive and egalitarian healthcare system, has been a leader in implementing VBHC from the beginning, a fact that was underscored in a 2016 global assessment of VBHC published by The Economist Intelligence Unit.
This paper looks at the ways in which Sweden has implemented VBHC, the areas in which it has faced obstacles and the lessons that it can teach other countries and health systems looking to improve the value of their own healthcare investments.

Breast cancer patients and survivors in the Asia-Pacific workforce
With more older women also working, how will the rising trend of breast cancer survivorship manifest in workplace policies, practices and culture? What challenges do breast cancer survivors face when trying to reintegrate into the workforce, or to continue working during treatment? How can governments, companies and society at large play a constructive role?
This series of reports looks at the situation for breast cancer survivors in Australia, New Zealand and South Korea. It finds that while progress has been made, more needs to be done, particularly in South Korea, where public stigma around cancer remains high.
The Cost of Silence
Cardiovascular diseases levy a substantial financial toll on individuals, their households and the public finances. These include the costs of hospital treatment, long-term disease management and recurring incidence of heart attacks and stroke. They also include the costs of functional impairment and knock-on costs as families may lose breadwinners or have to withdraw other family members from the workforce to care for a CVD patient. Governments also lose tax revenue due to early retirement and mortality, and can be forced to reallocate public finances from other budgets to maintain an accessible healthcare system in the face of rising costs.
As such, there is a need for more awareness of the ways in which people should actively work to reduce their CVD risk. There is also a need for more primary and secondary preventative support from health agencies, policymakers and nongovernmental groups.
To inform the decisions and strategies of these stakeholders, The Economist Intelligence Unit and EIU Healthcare, its healthcare subsidiary, have conducted a study of the prevalence and costs of the top four modifiable risk factors that contribute to CVDs across the Asian markets of China, Australia, Hong Kong, Japan, Singapore, South Korea, Taiwan and Thailand.
Download the report to learn more.
Enabling people to manage their health and wellbeing: Policy approaches to self-care
About this report
Enabling people to manage their health and wellbeing: Policy approaches to self-care is a report written by The Economist Intelligence Unit and sponsored by RB, a UK consumer goods company. The report considers the key elements and drivers for self-care, and examines the political and regulatory response across three global markets: the US, Europe and BRICS (Brazil, Russia, India, China and South Africa).
Related content

Value-based healthcare in Sweden: Reaching the next level
The need to get better value from healthcare investment has never been more important as ageing populations and increasing numbers of people with multiple chronic conditions force governments to make limited financial resources go further.
These pressures, along with a greater focus on patient-centred care, have raised the profile of VBHC, especially in European healthcare systems. Sweden, with its highly comprehensive and egalitarian healthcare system, has been a leader in implementing VBHC from the beginning, a fact that was underscored in a 2016 global assessment of VBHC published by The Economist Intelligence Unit.
This paper looks at the ways in which Sweden has implemented VBHC, the areas in which it has faced obstacles and the lessons that it can teach other countries and health systems looking to improve the value of their own healthcare investments.

Breast cancer patients and survivors in the Asia-Pacific workforce
With more older women also working, how will the rising trend of breast cancer survivorship manifest in workplace policies, practices and culture? What challenges do breast cancer survivors face when trying to reintegrate into the workforce, or to continue working during treatment? How can governments, companies and society at large play a constructive role?
This series of reports looks at the situation for breast cancer survivors in Australia, New Zealand and South Korea. It finds that while progress has been made, more needs to be done, particularly in South Korea, where public stigma around cancer remains high.
The Cost of Silence
Cardiovascular diseases levy a substantial financial toll on individuals, their households and the public finances. These include the costs of hospital treatment, long-term disease management and recurring incidence of heart attacks and stroke. They also include the costs of functional impairment and knock-on costs as families may lose breadwinners or have to withdraw other family members from the workforce to care for a CVD patient. Governments also lose tax revenue due to early retirement and mortality, and can be forced to reallocate public finances from other budgets to maintain an accessible healthcare system in the face of rising costs.
As such, there is a need for more awareness of the ways in which people should actively work to reduce their CVD risk. There is also a need for more primary and secondary preventative support from health agencies, policymakers and nongovernmental groups.
To inform the decisions and strategies of these stakeholders, The Economist Intelligence Unit and EIU Healthcare, its healthcare subsidiary, have conducted a study of the prevalence and costs of the top four modifiable risk factors that contribute to CVDs across the Asian markets of China, Australia, Hong Kong, Japan, Singapore, South Korea, Taiwan and Thailand.
Download the report to learn more.
A Renewed Commitment: Pakistan’s policy response to hepatitis B and C
Around 15m people are currently living with hepatitis B or C in Pakistan, the second highest in the world. Official data are more than a decade old—a national survey from 2007- 08 found a prevalence of 4.8% for HCV and 2.5% for HBV.
17306
Related content

Endgame: Egypt’s path to eliminating hepatitis B and C
The scale of infection with the hepatitis C virus (HCV) in Egypt was unlike any other country in the world—in 2015 an estimated 6.3% of the population was living with the virus. With a population of 93m at the time, that amounted to close to 6m people. In comparison, the prevalence of hepatitis B virus (HBV) was much lower, estimated at 1% of the total population.
The high prevalence of HCV in Egypt can be traced back to a programme that ran between the 1950s and 1980s to combat schistosomiasis, a water-borne parasitic disease that was endemic in the Nile Delta. Executed by the Egyptian Ministry of Health and Population with the advice and support of the World Health Organisation (WHO), 36m injections were administered to more than 6m people. Undertaken almost entirely with unsterilised and pre-used syringes and needles, the programme inadvertently transmitted HCV, which was not well known at the time. This, combined with weak infection control measures (such as quality controls for blood donations), led to high transmission rates and high prevalence.
Despite high HCV prevalence, the HBV-HCV co-infection rate was found to be just 0.06%, and the geographical distribution of the two infections differed markedly. Exposure to household members who are HBV positive has been found to be the main mode of transmission.
US$3.82bn Estimated economic burden of HCV in Egypt in 2015
The impact of HCV and HBV can be assessed on two fronts: the personal effects of the disease and its impact on economies in terms of employee productivity and direct medical costs. Chronic hepatitis is detrimental to a person’s quality of life, as they can experience fatigue and depression. There is a risk of developing progressive liver damage, which can lead to liver cancer or failure. HCV can increase the risk of type 2 diabetes and other health issues too. Both adversely impact employee productivity through disability and mortality. Specifically for HCV in Egypt, the economic burden was estimated at US$3.82bn in 2015. In terms of direct costs, HCV testing and treatment amounted to some 4% of total health expenditure in 2015 (over US$700m). The same study shows that treating over 300,000 individuals with HCV each year with antivirals could reduce its prevalence by 94% and liver-related deaths by 75% by 2030. Under this scenario, direct costs would be incurred, especially in the short-term to test and treat. But when indirect costs are taken into account, the intervention can be cost saving. Between 2015 and 2030, the estimated savings stand at US$4.6bn for direct costs and US$26.9bn for indirect costs.
Given the scale of the health issue, the response from the Egyptian government has been to craft and implement a national screening programme for chronic hepatitis, focusing on HCV, as well as treating those infected. The programme reached a milestone in May 2019, having screened 50m people across the country in six months. These efforts have been supplemented with infection prevention and control, ongoing surveillance and continued public education to sustain the positive health impact. As many countries in Africa and beyond battle against hepatitis B and C, there are vital lessons to learn from Egypt’s experience.
Reaching millions
As part of the Egyptian government’s commitment to address this health issue, they formed the National Committee for Control of Viral Hepatitis (NCCVH) in 2006, comprising representatives from the Ministry of Health and Population as well as liver and viral hepatitis experts.
The initial challenge was the state of public awareness. Three national studies had concluded that there were serious knowledge gaps in people’s understanding of hepatitis C. The response was to roll out a multi-channel mass education campaign, with clear messages for the public on risk factors (for those who have had surgery, blood transfusions or schistosomiasis injections), transmission modes (including reused syringes and shaving razors) and registering for testing.
In addition to other government initiatives to reach those in rural areas, Gamal Shiha, chairman of the board of trustees at the Egyptian Liver Research Institute and Hospital, and his colleagues at Mansoura University, launched the “Educate, Test and Treat” programme. Implemented across 73 villages, it was designed to educate people about viral hepatitis and start treatment rapidly. Education needs to be the first step, advises Dr Shiha. “If you go to a village without talking to the people and say ‘please come and be tested’, 50% will not come. But after we provide some information, people in the villages were welcoming.”
“When you cure everybody, there will be no transmission. We consider the massive treatment programme one of the pillars of prevention in addition to infection control.”
Dr Imam Waked, professor of hepatology, National Liver Institute
“We spent a lot on the media campaign but it was important to encourage people to come for testing,” says Wahid Doss, chairman of the NCCVH. The ambitious screening programme called “100 million healthy lives” cost between US$250m and US$300m and was partly funded from a loan by the World Bank. Of the 5m people estimated to have been living with HCV in 2014, 2.5m were treated between 2014 and early 2019, and 1.8m are expected to be treated by the end of 2019. As a result, the prevalence of HCV in Egypt is expected to decline from 7% to less than 1%. “When you cure everybody, there will be no transmission,” explains Imam Waked, professor of hepatology at the National Liver Institute at the University of Menoufiya and a member of the NCCVH. “We consider the massive treatment programme one of the pillars of prevention in addition to infection control.”
The 2-3% treatment failures would translate to about 50,000 patients who will need more specialised treatment that is not readily available in Egypt.
The last mile
At each stage from initial screening, there is a risk of drop-off as people fail to come back for further tests or complete treatment. The problem is most acute in rural areas, given long distances from testing and treatment centres and high levels of poverty. Layer this with cultural impediments (particularly among women, who are reluctant to leave behind their obligations at home to travel large distances) and it is easy to see why drop-off-rates can be high. To reduce the number of visits required, the “Educate, Test and Treat” programme led by Dr Shiha found a way to offer all the tests required to initiate treatment on a single day.
Going forward, a key challenge will be dealing with treatment failures. Even in the best scenarios, cure rates are between 97-98%. The 2-3% treatment failures would translate to about 50,000 patients who will need more specialised treatment that is not readily available in Egypt. To protect against transmissions from treatment failures, adoption of infection prevention and control measures can be effective.
A holistic approach
To eliminate HCV as a public health threat by 2023 requires a well-rounded approach beyond the current mass-screening and treatment campaign. These include a range of infection prevention and control policies, funded through a combination of government resources and a loan from the World Bank given to upgrade Egypt’s health system, explains Dr Waked.
To incentivise patients to report on treatment outcomes, the Ministry of Health and Population offered a certificate of cure, which was required to secure employment abroad. This improved reporting rates dramatically to 67%, from 25%
Injection safety, which addresses an important mode of transmission for viral hepatitis, has improved over the years. A recent assessment by the WHO found that all public-sector hospitals and 98% of private-sector hospitals used needles and syringes taken from a sterile packet or fitted with caps. To enhance this, healthcare facilities across Egypt will be required to use only auto-disabled syringes by July 2020. Greater adoption of best practice around preparing injections in a dedicated area and cleaning of needles are required.
To further strengthen infection prevention and control, blood banks will be conducting more stringent analysis of blood donations. In addition, the WHO’s national standards for blood transfusion services are being disseminated across Egypt to ensure that protocols for safe transfusion of blood are followed, complemented by efforts to improve regulatory oversight. This entails the formation of a national blood authority and revising the blood safety law.
Prevention measures for HBV have been in place for decades. Egypt began vaccinating infants in 1992, although testing of pregnant women has not been consistent. One study concludes that the existing vaccination programme provides adequate protection. From early 2019, hospitals have been administering the “birth dose”, delivering the first dose of the vaccine within 24 hours after birth (previously the first dose was given two months after birth). As part of the screening and treatment programme for HCV, vaccinations for HBV were also provided.
For further analysis of progress on eliminating HBV and HCV, the government needs to close the reporting gap. To incentivise patients to report on treatment outcomes, the Ministry of Health and Population offered a certificate of cure, which was required to secure employment abroad. This improved reporting rates dramatically to 67%, from 25%; follow-ups over the phone pushed the rate higher, to 75%. Experts we interviewed suggest that all public and private facilities should be reporting into the same database, with a clear link to individual patient IDs.
Sustaining the positive health impact
Looking ahead, health workers and people themselves must remain vigilant for symptoms of viral hepatitis and risk factors for transmission. But the government in Egypt must continue to provide the tools necessary, including frequent training for health workers as conditions evolve and an extended public education programme.
The screening programme accelerated the efforts to reach the millions who were infected, justified by the scale of the health issue. “It required estimating the magnitude of the problem, establishing treatment centres around the country and securing the political will and financing to provide affordable treatment to the people,” describes Dr Doss. But this must be complemented with effective infection prevention and control policies, including injection and blood safety, to reduce transmission. Dr Shiha concludes, “The government’s direction is very good and the commitment makes me happy. My dream is an Egypt, and a whole world, free of hepatitis C and B.”
Downlaod Arabic PDF here

Taking aim: The policy response to viral hepatitis in Uganda
“What you don’t know can’t hurt you” doesn’t apply to Uganda’s health challenges with hepatitis B and C. Data on prevalence are sparse, particularly for the hepatitis C virus (HCV). Based on small-scale studies, prevalence of HCV is estimated at 1-2% of the total population, says Ponsiano Ocama, chair of the department of medicine and academic hepatologist at Makerere University College of Health Sciences. Estimates for the hepatitis B virus (HBV) are better but based on an HIV impact assessment survey conducted in 2016. It places prevalence at 4.3% of the population aged between 15 and 49 years, with the highest prevalence in the northern region of the country.
There is evidence, albeit limited, that viral hepatitis is a growing health challenge in Uganda. Screening of blood donations for HBV and HCV has thus far been the primary source for identifying infections. According to a government-issued press release, Uganda Blood Transfusion Services has reported an increase in HBV found in blood donations from 1.9% in fiscal year 2012/13 (July-June) to 2.3% in 2016/17, confirming the higher prevalence in the northern and eastern parts. In addition, researchers have recently discovered three new strains of HCV in Uganda.
Importantly though, these figures exclude prevalence in children. In Uganda, HBV is mainly acquired before the age of five, explains Dr Ocama, believed to largely be the result of mother-to-child transmission. Among adults, modes of transmission are thought to include pre-used needles or shared blades, arising from skin scarification practices prevalent in some parts of the country.
At the Uganda Cancer Institute, the largest public-sector cancer institute in East Africa, “out of 280 liver cancer patients in 2018, 80-90% were attributable to viral hepatitis”.
Dr Olaro Charles, director curative services, Ministry of Health, Uganda
The health and financial burden of hepatitis B and C on patients and the government can be high, but with no robust estimates of the economic burden, the severity in Uganda is difficult to assess. One outcome that experts we interviewed emphasise is that chronic hepatitis can progress to liver cancer. At the Uganda Cancer Institute, the largest public sector cancer institute in East Africa, “out of 280 liver cancer patients in 2018, 80-90% were attributable to viral hepatitis,” explains Dr Olaro Charles, director curative services at the Ministry of Health. Addressing chronic hepatitis, he argues, is a way to address the cancer challenge too. Policymakers should assess the short-term costs to test and treat viral hepatitis against the future savings in healthcare expenditure if fewer people require cancer care.
In 2014 the government acknowledged that hepatitis is a serious health concern, making a public declaration to address it. The policies, however, focus almost exclusively on HBV with little or no mention of HCV. In this article, we examine the state of the policy response and priority areas for the future, as Uganda aims to meet this health challenge.
US$3m Amount earmarked in the annual government budget to tackle HBV in Uganda.
Closing the information gap: Reporting and public awareness
An estimated US$3m of the annual government budget has been earmarked to tackle HBV in Uganda. In 2015 they launched a screening and treatment programme exclusively for HBV, targeting those above the age of 15. Those who test negative are given vaccinations, as a preventative measure. This effort started in the north, where the prevalence is very high, followed by east Uganda, with the aim of covering the whole country.
Information gathered as part of the programme will be valuable, providing more data on the prevalence of HBV than what is currently available. This will be important for completing the government’s strategic plan to tackle hepatitis, which is currently under development, and measuring progress in subsequent years. To strengthen its reporting system, in early 2019 the Ugandan government was given access to the Global Hepatitis Reporting System, which was created by the World Health Organisation (WHO). As part of this, various stakeholders in the healthcare system received two days of training by the WHO. Lessons on best practice learned over the course of the African Hepatitis Summit in Kampala in June 2019 may inform the strategy as well.
“Some people think that hepatitis is transmitted like the Ebola virus. So, whenever someone is identified in the community as having hepatitis, the whole community may exclude this person, even in families.”
Kenneth Kabagambe, executive director, National Organisation for People Living with Hepatitis B
In the absence of a formal framework, nongovernmental organisations (NGOs) such as the National Organisation for People Living with Hepatitis B (NOPLHB) have been very active in Uganda. They advocate for the rights of hepatitis patients and improving diagnostic and clinical services for patients. Importantly, they help to raise public awareness about HBV prevention, care and support services.
Resistance to testing for hepatitis stems from stigma and misinformation. Kenneth Kabagambe, the executive director of NOPLHB, says, “Some people think that hepatitis is transmitted like the Ebola virus. So, whenever someone is identified in the community as having hepatitis, the whole community may exclude this person, even in families.” A wider public awareness programme can help to correct misinformation, strengthen prevention practices and encourage people to get tested and treated. Adopting a multi-channel approach—through television, radio and billboards—could help reach the masses.
The building blocks to prevent, test and treat
Experts we interviewed point to health worker training as a priority going forward. Health workers have received training as part of the government’s wider efforts to improve injection safety, but more specific training on viral hepatitis is needed. “At the moment, we still have some health workers who don’t understand what hepatitis B and C is,” states Mr Kabagame. Dr Ocama concurs, explaining that there are challenges with the quality of training programmes. These need to be structured around an approved curriculum, enabling health workers to better identify at-risk patients and effectively treat those infected. To this end, the government is developing treatment guidelines. Broader protections include policies announced in 2014 requiring all health workers to be vaccinated for hepatitis B.
“We are now trying to see the feasibility of having HBV services integrated to the HIV setting. And then, if it is feasible, we are trying to assess what kind of additional funding will be required.”
Dr Ponsiano Ocama, chair of the department of medicine and academic hepatologist, Makerere University College of Health Sciences
To tackle the prevalence of HBV among children, the government introduced a vaccination programme for infants at six weeks after birth. Based on one study in Uganda, the programme seems to be effective: among 73 children who had been vaccinated, none were infected with HBV. To strengthen this, Mr Kabagambe advocates for the “birth dose”, under which infants receive the first dose within 24 hours after birth, in line with WHO recommendations. To safeguard against mother-to-child transmission, hepatitis testing should be made mandatory for pregnant women, asserts Mr Kabagambe.
Another gap in the system in Uganda is the completion rate of the vaccination programme among those who test negative. At present, 92% of those eligible for the hepatitis B vaccine receive the first dose, 68% receive the second dose and only 33% receive the third dose. Educating patients on the importance of vaccinations and completing treatment is part of the solution, and should be a core pillar of the country’s strategy for preventing and reducing transmission. Another part of the solution will be driving operational efficiency, making these subsequent doses more accessible to patients living in remote areas in particular.
The finance function
Across the system, improving access to testing and treatment has two components, both rooted in financial constraints. The first is that patients are required to pay for some tests before starting treatment. This is resulting in delayed diagnosis, explains Mr Kabagambe: “We are seeing that most of the patients who are infected are going to hospitals when they are at the end stage of the disease, when it is very advanced.”
The second impediment to testing and treating is that diagnostic equipment, especially in rural areas, is often made available through donor funds, which do not take into consideration maintenance and other recurrent costs.
To tackle the financing challenge, opportunities to integrate hepatitis services with HIV programmes could be leveraged. There are many similarities between HIV and hepatitis in terms of transmission, disease progression, diagnostic and monitoring equipment required, and in some cases the treatment too. Globally, between 5% and 20% of people living with HIV are also infected with HBV. “We are now trying to see the feasibility of having HBV services integrated to the HIV setting,” says Dr Ocama. “And then, if it is feasible, we are trying to assess what kind of additional funding will be required.”
The Global Fund to Fight AIDS, TB and Malaria now allows applicants to include work to address HIV comorbidities such as hepatitis in their funding requests. However, such requests would need to come from the country’s allocated funding for HIV, which already falls short of what is required in the case of Uganda. That may explain why funding for hepatitis has so far relied entirely on domestic sources, but this does not preclude opportunities for funding integration in the future.
Looking ahead
The Ministry of Health is taking some positive steps to address hepatitis in Uganda, with a dedicated budget and staff as well as the development of a strategic plan. But the plan must take into consideration various facets of the health issue.
Enhancing reporting from the screening programme under way as well as a planned nationwide survey will provide much-needed data on HBV and HCV prevalence. This will enable the government to craft evidence-based policies and plans with specific targets. Without plans and targets, it will be difficult to assess progress and the degree of alignment with WHO recommendations.
Emphasis on health worker training and providing treatment guidelines will be critical for the successful implementation of the strategy. In addition, the government can leverage the expertise of active NGOs in the country and build on their efforts to raise public awareness and advocate for patients’ rights and services. Broader education efforts to erase the stigma attached to these curable and preventable diseases will be an important driver of success as Uganda works towards the WHO goal of eliminating hepatitis B and C by 2030.
Diagnosing Healthcare in the GCC
Vast oil wealth in the Gulf has led to lifestyle changes which, in turn, have given rise to increased incidence of non-communicable diseases (NCDs). Healthy traditional diets have been almost entirely replaced by a high-sugar, low-nutrient diet. Tobacco smoking has been taken up by men, women and children. An active lifestyle, which came naturally to the self-sufficient nomadic forebears of Gulf Arabs, has largely been replaced by desk-bound jobs. This has led to an evolution in the disease profile of the region from a preponderance of infectious diseases to chronic diseases spanning obesity, diabetes, heart disease and cancer.
The growing prevalence of these lifestyle-related diseases also has wider economicimplications. It is therefore essential that these health issues are diagnosed and tackled before they progress and become chronic if the region is to develop a well-educated, skilled and diversified workforce and thereby achieve its economic potential. To do this, healthcare systems in the region need to adapt to changes in the disease profile. This paper examines the current state of healthcare delivery in the Gulf Co-operation Council (GCC), with a focus on the diagnostic process, and identifies strategies for the way forward.
